At a high-level, patient waits are reduced when patients are scheduled at a time when their care teams will be available to treat them. However, in reality, Patient Scheduling is far more complex. Care Teams strive to create schedules that are always full (to maximize revenue in Fee-For-Service reimbursement models) despite no-shows, cancellations, late patients, and a mix of short and long patient cycle times, and end at a reasonable hour.
For a typical clinician, there are over a Google possible ways to schedule patients in a given day. The vast majority of clinics schedule patients in a way that maximize revenue. A smaller percentage also ensure a reasonable end to the workday. Very few maximize revenue, respect clinician’s workdays, and maximize patient experience – this is an incredibly difficult mathematics problem to solve without the right data and software tools.
RTLS was clinically validated by the Dana Farber Cancer Institute (1) as the missing piece in building schedules that achieve success for revenue, clinician experience, and patient experience. They recognized that EHR data alone was an insufficient method for finding optimal schedules out of these Google possibilities and that RTLS was the key to quickly and accurately building clinician and patient-friendly schedules. There are three elements to this problem:
Kadish, Sarah, MS. “Transforming Process Improvement through RTLS Data.” HIMSS15 Annual Conference & Exhibition, April 14, 2015.
Vanderbilt Urology is a worldwide leader in Urological Care and a Top 10 Urology center in the country. Their clinic recognized that Apprentice Health was the pioneer of IoT workflow sensing, activity based costing, and predictive Patient Scheduling for ambulatory clinics (2).
Early on in the partnership, the two teams agreed upon the necessary ingredients for high-performance patient scheduling and debunked many common patient scheduling myths.
Sensor Data over EHR time-stamp data. Like many clinics across the country, Vanderbilt Urology recognized that their existing EHR data was insufficient to optimize their processes. Sensor data accurately and passively maps out all the process flows. EHR time-stamp data, on the other hand, is incomplete – it does not typically reflect the actual flow of operations, is difficult to scale, and is not real-time. While a few clinics across the country have had minor successes using EHR time-stamps, Machine Learning, and simulation – most have not due to poor data quality. Moreover, EHR time-stamp based models can’t accurately power predictive staffing, real-time workflow orchestration, or activity-based costing applications.
The future of healthcare operations will rely on passive sensing, not manual data-entry. The future of healthcare is ambient and enriched by sensors – finally freeing clinicians and patients from being tethered at all times to the EHR.
Personalized Scheduling over One-Size Fits All Scheduling. Many of the ambulatory executives we have spoken to across the country are currently attempting to bring standardization to their patient access strategies. While standardization of some elements of patient access is vital, standardization of the timing and cadence of the template slots themselves is a recipe for both poor patient experience and clinician push-back.
Clinicians want schedules that reflect how their Care Teams work together, respect their workflow patterns, and provide patients a consistent, high-quality experience. One-Size fits all scheduling results in missed revenue and poor patient experience, as these schedules don’t reflect operations truth.
Maintain Current Clinician Workflows over Complete Overhaul. Clinician schedules can be political and reflect years of negotiated history on ways to share procedure space, staff, and other resources. Predictive scheduling systems must respect these constraints and find other ways to improve the process.
Comprehensive Solution over Point Solution. Successful patient schedule strategies can’t rely on only no-show prediction and cancellation dynamics. While these are very important variables, the picture is far more complex. For example, most common no-show prediction models will actually increase patient wait times if not used in combination with data on patient arrival times, wait times, team dynamics, and interaction times. Many hospitals are now discovering this the hard way. Talk to us and we’ll teach you why.
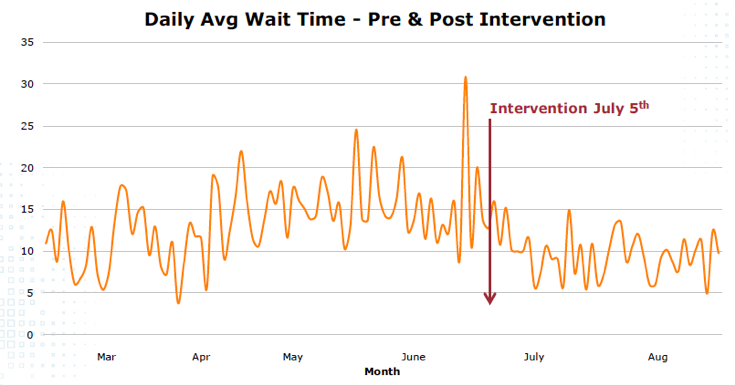
Vanderbilt Urology was correct in promoting these scheduling principles. After implementing Apprentice Scheduling Core templates, patients experienced a 40% reduction in wait times.
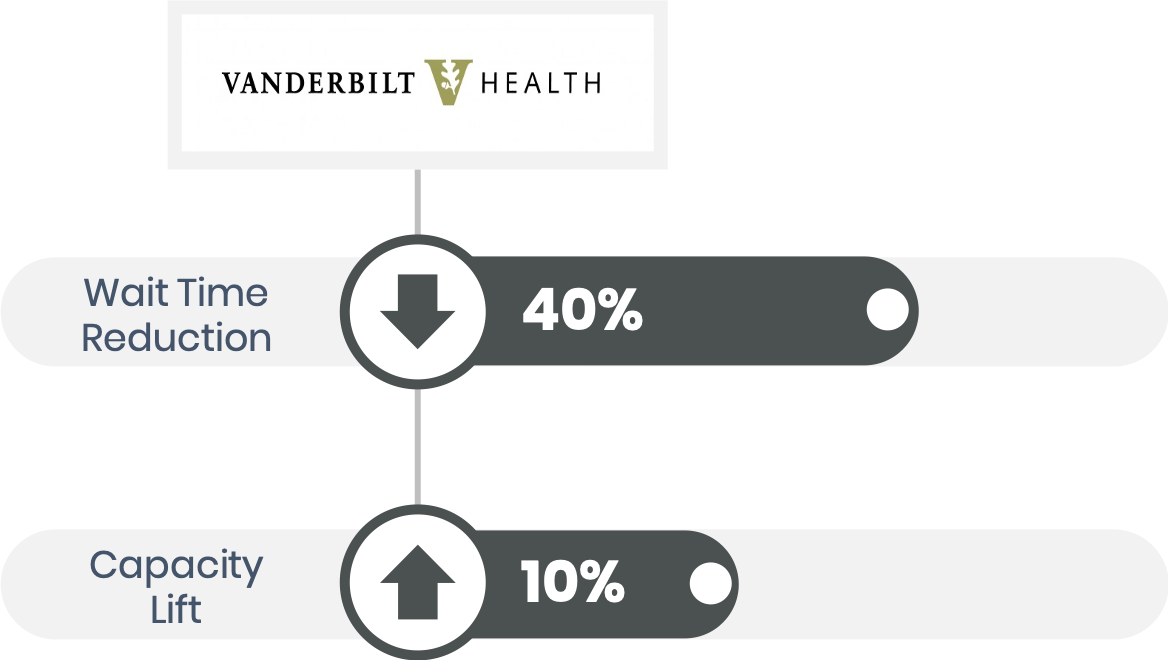
Apprentice Health recognized that a commercial Patient Scheduling solution was needed that leveraged less expensive IoT infrastructure and advances in computing.
Over our first two years as a company, we built the needed RTLS, process mining, simulation, and data science software needed to quickly scale better patient scheduling across the globe.
We believe these Apprentice Health modules represents the largest ROI of any software intervention in outpatient medicine today. Individual clinicians do not need to see more patients to achieve revenue gains.
And we’re just getting started. This was all done without EHR integration to limit any typical IT approval delays. Incorporation of medical history and demographic information into the predictive models enables an even higher degree of predictive accuracy that will further decrease patient wait times and improve patient experience.
Apprentice Health is on track to optimize over 1,000,000 patient visits by the end of 2020. We’ve partnered with some of the leading hospitals in the country and are now looking to partner with healthcare champions passionate about operations, patient experience, and building a sustainable healthcare system.