What if you could increase your revenue by 10-20% by treating more patients and reduce physician burnout at the same time? Better allocation of exam room space is the key to achieving these goals.
Leading ambulatory clinics ensure that their clinics achieve profitability by making sure that exam rooms are always being productively used and patients remain satisfied. However, it turns out that even with a focused effort, the vast majority of clinics still have very low rates of productive exam room utilization.
There are three elements to this problem:
In all three of these scenarios, patients spend too much time waiting in exam rooms, taking up space that another care team could use to treat other patients.
The Dana Farber Cancer Institute (DFCI) in Boston recognized that despite their best efforts, their productive exam room utilization was only at 50%, despite clinicians feeling that rooms were always occupied and patients waiting an average of 15 minutes to room. Compounding the problem, DFCI needed to combine two clinic facilities and absorb a 10% increase in patient volume while using the combined facility’s existing capacity.
DFCI leadership installed a Real-Time Locating System (RTLS) and partnered with academics to use this data to make better use of existing space.
By using RTLS data, DFCI reduced average wait time to exam room despite a simultaneous increase in the average appointment volume during the post-intervention period. DFCI leadership installed an RTLS and partnered with academics to use this data to make better use of existing space.
They developed a data science module that used real-time information to inform the medical assistants when to place patients into rooms and which rooms to place them in. Clinicians would no longer be assigned exam rooms under a ‘fixed’ allocation policy, and instead share among a pool of available exam rooms. Fixed exam room allocation policies are known to be sub-optimal, however, are typically deployed given the lack of a Real-Time Locating System.
However, at the DFCI, clinicians could easily find their patients due to RTLS information shown on LCD screens. After this intervention, their clinicians were happier with the room-sharing strategy than the ‘fixed’ room strategy.
In the end, the combined intervention of reducing patient wait times and dynamic room-sharing was game-changing for DFCI. Every stakeholder benefited.
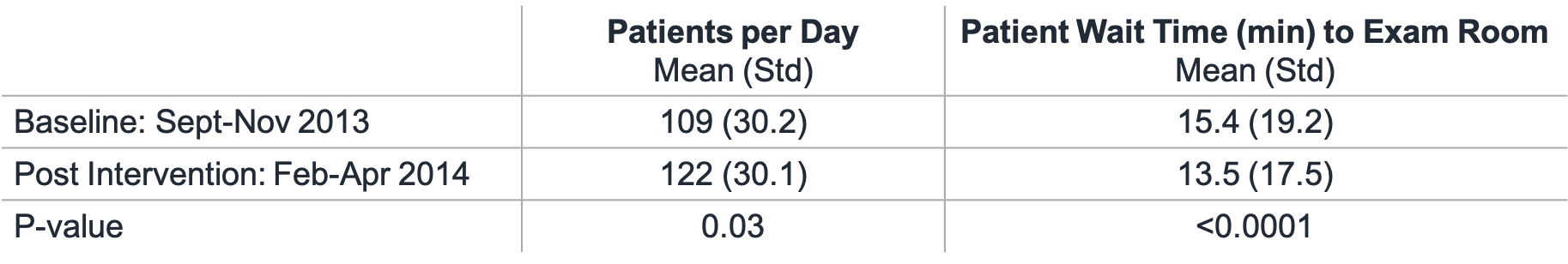
Beth Overmoyer, Sarah Kadish, Courtney Haskett, Kendall Sanderson, Jim Benneyan, Christine Reilly, Lillian Vitale Pedulla, Linda Brown, Kristen Camuso, and Craig A. Bunnell. Journal of Clinical Oncology 2014 32:30_suppl, 157-157.
"In the end, we saw a 10 percent increase in capacity without changing the number of rooms we had. Because of the workflow changes we made, we were essentially able to add two rooms to each floor, just by using that real estate more efficiently."
- Dr. Craig Burnell (CMO, DFCI)
Apprentice Health takes a similar approach to the DFCI, but with a modern software architecture and less expensive Bluetooth Low Energy (BLE) badges. We've made it easy to install the necessary RTLS, helping clinics reduce patient wait times without prolonging the length of day and increase patient access by enabling fluid room sharing.
Now clinics across the country can take advantage of better room allocation, freeing up space for an additional 10-20% of patients per day.
We believe Apprentice Health modules represent the largest ROI of any software intervention in outpatient medicine today. Individual clinicians do not need to see more patients to achieve revenue improvement.